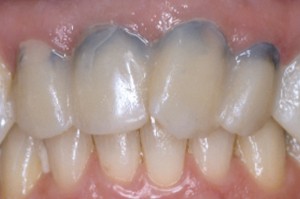
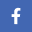Many clinicians encounter the dark staining of a patient’s tissues after the use of a hydrophobic cement. Fortunately, this is a challenge that is treatable, and even better, preventable! First, let’s take a look at the reasons behind why this pesky staining occurs in the first place.
It’s all about the chemistry. Non-sealing cements allow saliva and bacteria to move between the temporary and preparation. Coagulum within cut tissues is a source of iron, which reacts with the hydrogen sulfide gas (rotten egg gas, H2S) produced by anaerobic bacteria in this septic environment. The reaction yields ferric sulfide—the harmless, yet annoying dark surface stain shown in the photo below.
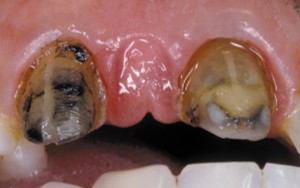
This staining can also occur, to a lesser degree, from the natural iron in the blood. Additionally, non-sealing provisionals are problematic, as the presence of saliva and/or bacteria removes the smear layer within one week, opening tubules to bacteria.
One way to prevent this from occurring is to use an antimicrobial temporary cement (like ZOE), which leaks, but at least prevents bacterial growth, hence no H2S and no formation of ferric sulfide. However, there’s an even better way to go about it.
The most sure-fire way to prevent staining under provisional cement is to use a sealing, hydrophilic, non-eugenol, polycarboxylate, paste-to-paste cement like Ultradent’s UltraTemp.
UltraTemp
As an extra precautionary measure (as similar staining can still occur if contamination is on the preparation prior to bonding) scour and/or etch as needed prior to DBA application. For scouring, we recommend using Consepsis Scrub with the STARbrush.
Consepsis Scrub

STARbrush